Abriendo camino: Del diagnóstico a un nuevo comienzo
Un diagnóstico de cáncer colorrectal le da vuelta al mundo. La cirugía que sigue—a menudo una resección abdominoperineal (APR) o procedimiento de Hartmann—salva vidas. Pero también significa aprender a vivir con una colostomía: una abertura creada quirúrgicamente (estoma) en su pared abdominal a través de la cual su colon ahora se vacía en una bolsa.
Si está leyendo esto, probablemente acaba de recibir su diagnóstico, o está ayudando a alguien que lo tiene. El shock es real. La incertidumbre es válida. Pero aquí está lo que muchos ostomates descubren una vez que pasan el ajuste inicial: la vida con colostomía no es la limitación que podría temer. En muchos sentidos, es más liberadora de lo que esperaría.
A diferencia de otros tipos de ostomía, los sobrevivientes del cáncer colorrectal con una colostomía tienen acceso a una técnica revolucionaria llamada irrigación—un método que puede significar la diferencia entre usar una bolsa todos los días y disfrutar de largas rachas de libertad, nadar sin preocupación y hacer ejercicio sin inquietud. Esta guía lo guía a través de todo lo que necesita saber: cómo funciona la colostomía, por qué importa la ubicación, cómo la irrigación puede transformar su calidad de vida, y cómo recuperar su confianza después de la cirugía.
¿Qué es una colostomía?
Una colostomía es una abertura creada quirúrgicamente (llamada estoma) en su colon que se lleva a la superficie de su pared abdominal. Su colon—el intestino grueso—normalmente absorbe agua de las heces y controla el tiempo de los movimientos intestinales. Después de la cirugía de colostomía, esta abertura evita la porción de su colon que estaba enferma o dañada, y las heces ahora pasan a través del estoma hacia una bolsa usada en el exterior de su cuerpo.
Aquí está lo que hace única la colostomía: la salida es formada. A diferencia de los pacientes con ileostomía (cuya salida es líquida porque evita todo el colon), los pacientes con colostomía pasan heces que son más cercanas a la consistencia normal. Esta diferencia fundamental determina todo sobre cómo manejará su colostomía día a día, y es una razón por la cual muchos ostomates encuentran que la colostomía es más fácil de manejar que otros tipos de ostomía.
Su estoma es rosa o rojo (como el interior de su boca) y probablemente se reducirá a su tamaño permanente dentro de 4 a 6 semanas después de la cirugía. It has no nerve endings, so you won’t feel pain when it touches something—though you’ll develop a sensation of pressure or fullness when output is coming, which helps you recognize when your pouch needs emptying.
¿Dónde en el colon? Cómo la ubicación cambia todo
No todas las colostomías se crean iguales. La ubicación de su estoma en el colon afecta dramáticamente la consistencia de su salida, con qué frecuencia necesitará vaciar su bolsa, y críticamente—si es candidato para la irrigación. Comprender la ubicación de su estoma es esencial para manejar su colostomía de manera efectiva.
Ubicación de colostomía y consistencia de salida
Colostomía ascendente (lado derecho del abdomen): La salida es pastosa a líquida. Salida más frecuente. Ubicado cerca del ciego.
Colostomía transversa (a través del abdomen superior): La salida es pastosa. Frecuencia moderada. Menos común.
Colostomía descendente (lado izquierdo del abdomen): La salida es formada. Menos frecuente. La irrigación a menudo es posible.
Colostomía sigmoidea (abdomen inferior izquierdo): La salida es formada. Salida menos frecuente. Mejor candidato para irrigación. Tipo más común.
La colostomía sigmoidea es el estándar de oro—la salida suele ser formada (heces casi normales), y los movimientos intestinales son predecibles. Muchos ostomates sigmoideos pueden establecer rutinas de irrigación que les permiten pasar la mayoría del día sin bolsa. Esto es un cambio de juego para la calidad de vida.
Si su colostomía se ubica más arriba en el colon (ascendente o transversa), su salida será más pastosa o líquida, y probablemente necesitará usar una bolsa continuamente. Eso no hace que su colostomía sea menos manejable—simplemente significa que su rutina se ve diferente, e irrigación típicamente no es una opción para usted.
Tipos de colostomía
Más allá de la ubicación, las colostomías se clasifican por tipo según cómo se realizó la cirugía. Existen tres tipos principales:
| Tipo de colostomía | Qué es | Reversibilidad | Razón común |
|---|---|---|---|
| Colostomía terminal | Un extremo del colon llevado a la superficie de la piel. Intestino enfermo removido o no funcional. | Permanente (a menos que se planee reversión) | APR para cáncer rectal, enfermedad de Crohn extensa, poliposis familiar |
| Colostomía de asa | Asa de colon sacada a la superficie; ambas ramas abiertas al abdomen. Generalmente temporal. | A menudo temporal (reversible) | Obstrucción intestinal, desviación de emergencia, trauma |
| Colostomía de doble barril | Dos estomas separados: proximal (activo, pasa heces) y distal (recibe mucus del intestino no utilizado). | Generalmente temporal (reversible) | Procedimiento de Hartmann; diverticulitis; trauma |
Si tuvo un procedimiento de Hartmann (el más común para el cáncer colorrectal donde se extirpa el recto), tiene una colostomía de doble barril con la posibilidad de reversión en el futuro. El estoma proximal es por donde pasan las heces; el estoma distal puede descargar pequeñas cantidades de mucus. Cubriremos la reversión en detalle más adelante.
Por qué podría necesitar una colostomía
El cáncer colorrectal es la razón principal para la colostomía, pero no es la única. Aquí está lo que lleva a las personas a la cirugía de colostomía:
- Cáncer colorrectal — La razón #1. Los cánceres del colon o recto requieren la extirpación del segmento afectado. Una resección abdominoperineal (APR) extirpa el recto y el ano, requiriendo una colostomía permanente. Se puede realizar un procedimiento de Hartmann como una medida temporal, con la posibilidad de reversión posterior.
- Poliposis adenomatosa familiar (PAF) — Condición genética hereditaria que resulta en cientos de pólipos; la colectomía profiláctica a menudo se recomienda para prevenir el cáncer.
- Enfermedad diverticular — La diverticulitis grave y recurrente (inflamación de pequeñas bolsas en el colon) puede requerir colectomía y colostomía para prevenir la perforación potencialmente mortal.
- Enfermedad de Crohn — La enfermedad de Crohn grave e intratable que afecta el colon puede requerir extirpación quirúrgica y colostomía. (Nota: La colitis ulcerosa, que afecta solo el colon y el recto, típicamente lleva a ileostomía, no colostomía, porque se extirpa todo el colon.)
- Obstrucción intestinal — La obstrucción aguda por cáncer avanzado, estenosis u otras causas puede requerir colostomía de emergencia como desviación.
- Perforación intestinal o trauma — El intestino perforado por trauma, isquemia u otros eventos agudos puede requerir colostomía.
Independientemente de por qué necesita una colostomía, el ajuste adelante es real—pero manejable, e cada vez más normal con millones de ostomates en todo el mundo viviendo vidas plenas y activas.
Irrigación de colostomía: La técnica que lo cambia todo
Esta es la sección que distingue la colostomía de todos los otros tipos de ostomía. La irrigación es una técnica única para la colostomía—los pacientes con ileostomía y urostomía no pueden irrigar porque la salida es continua e impredecible. Pero los pacientes con colostomía, especialmente aquellos con colostomías sigmoideas o descendentes, pueden usar irrigación para ganar un control notable sobre los movimientos intestinales y, en muchos casos, eliminar la necesidad de usar una bolsa durante la mayoría del día.
¿Qué es la irrigación de colostomía?
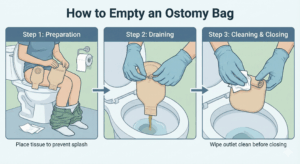
La irrigación de colostomía es el lavado intencional de agua en su estoma para desencadenar un movimiento intestinal planeado. Es esencialmente recrear el control que su colon solía tener: en lugar de que las heces pasen aleatoriamente durante el día (en una bolsa que está usando), usted instila agua una vez al día según un horario que funciona para usted—y las heces pasan en una ventana predecible, en el inodoro.
El proceso utiliza un kit de irrigación especial: una bolsa de agua tibia, una punta en forma de cono que se ajusta suavemente sobre el estoma (evitando que el agua salpique), tubing, y una tapa de estoma o un pequeño apósito. Usted instila aproximadamente 500-750 mL de agua (tibia, no caliente), se relaja, y deja que la gravedad y el reflejo natural de su colon hagan el trabajo. La salida típicamente viene dentro de 30-60 minutos, y luego puede usar una pequeña tapa o ninguna bolsa en absoluto para el resto del día.
¿Quién puede irrigar?
No todos los que tienen una colostomía son candidatos para la irrigación, pero muchos lo son—y vale la pena discutirlo con su cirujano colorrectal o terapeuta enterostomal (enfermera ET) temprano en la recuperación:
- Sigmoid or descending colostomy: Formed output and predictable bowel reflexes make irrigation successful. Ascending colostomy patients are rarely candidates because output is too liquid.
- Adequate manual dexterity: You need to manage the irrigation equipment safely. Arthritis, tremors, or limited hand strength may make it challenging.
- Adequate visual acuity: You need to see your stoma to position the cone correctly.
- Good cognitive function: Understanding the routine and troubleshooting issues is essential.
- Healthy stoma: No prolapse, severe stenosis, or other complications that would interfere with the cone placement.
- No absolute contraindications: Loop colostomies, familial polyposis with internal pouch complications, or certain inflammatory bowel disease patterns may not be suitable for irrigation.
How to Irrigate: Step-by-Step
The Irrigation Process
- Gather supplies: Irrigation kit (bag, tubing, cone), warm water (500-750 mL), lubricant, privacy, and time (allow 45 minutes to an hour).
- Sit on the toilet or in a special irrigation seat: You want to be positioned so output goes directly into the toilet. Some people remove their pouch entirely; others sit on an irrigation seat designed for colostomies.
- Hang the water bag: At about shoulder height or slightly above, so gravity delivers the water gently.
- Lubricate the cone: Use a small amount of water-soluble lubricant on the tip.
- Gently insert the cone: Angle the cone slightly and guide it into your stoma. The cone should fit snugly but never force it. You’ll feel gentle resistance—that’s normal.
- Open the clamp: Water flows in slowly (takes 5-10 minutes to instill 500-750 mL).
- Remove the cone and wait: Most output comes within 20-30 minutes, but allow 30-60 minutes total. Sit close to the toilet or use an irrigation seat.
- Clean and dry: Rinse your stoma gently, pat dry, and apply a fresh pouch or stoma cap.
The Benefits of Irrigation
If you’re a candidate and willing to establish a routine, irrigation offers life-changing benefits:
- Pouch-free freedom: Once you’ve irrigated, you can wear a small stoma cap or breathable cover instead of a full pouch for 20-24 hours. No bulk, no noise, no worry about leaks during that period.
- Control and predictability: Bowel movements happen on your schedule, not randomly. This is profound for confidence and planning.
- Improved swimming and exercise: With irrigation established, you can swim, run, or do intense exercise knowing your colon is empty and won’t output unpredictably.
- Reduced odor: Controlled, predictable output means fewer surprises and less odor anxiety.
- Psychological empowerment: For cancer survivors especially, irrigation represents reclaiming control over your body.
- Cost savings: Using stoma caps instead of pouches reduces long-term supply costs (though training and initial supplies are an investment).
Risks and Contraindications
Irrigation is generally safe, but some risks exist—and some situations make it inappropriate:
- Perforation: Extremely rare, but aggressive cone insertion or high water pressure can perforate the colon. Gentleness is key.
- Mucosal prolapse or bleeding: If your stoma prolapses (tissue herniates through the stoma), irrigation may exacerbate it.
- Dehydration or electrolyte imbalance: In rare cases, particularly high irrigation volumes can affect fluid balance. This is more theoretical than practical.
- Loop colostomy: Irrigation through a loop stoma can be challenging and is generally not recommended.
- Uncontrolled Crohn’s disease: If your Crohn’s is active or you have extensive small-bowel disease, irrigation may not be successful.
- Strictures: A severely narrowed stoma opening may prevent the cone from being placed safely.
Getting Started: Timeline and Expectations
Most people begin irrigation 4-6 weeks after surgery, once the stoma has settled and you’ve adjusted to basic pouch management. Your ET nurse will teach you the technique—this education is crucial and often covered by insurance. Initial attempts may feel awkward or produce unpredictable results, but within 2-4 weeks, most irrigating ostomates establish a reliable routine.
The first few irrigations might produce little to no output; the bowel needs time to adapt to the stimulus. Patience is essential. By week 3-4, most ostomates see predictable results and can confidently plan their day around the irrigation window.
Colostomy vs Ileostomy: The Real Differences
If you’re comparing colostomy to other ostomy types, here’s how they differ:
| Aspect | Colostomy | Ileostomy | Urostomy |
|---|---|---|---|
| Output Type | Formed stool (varies by location) | Liquid, pasty (continuous) | Urine (continuous) |
| Frequency | 1-2 times daily (or irrigated) | 5-8 times daily or continuous | Continuous throughout day/night |
| Pouch Wear | Usually 3-5 days; can be pouch-free with irrigation | Every 3-5 days; always worn | Every 1-2 days; always worn |
| Irrigation Possible? | Yes (sigmoid/descending only) | No | No |
| Diet Flexibility | High (colon absorbs water) | Moderate (no colon to absorb water) | High (not digestive) |
| Odor Control | Moderate (formed stool, odor-controlling foods work) | Higher (liquid output, more odorous) | Moderate (urine has characteristic smell) |
| Common Causes | Colorectal cancer, diverticulitis, Crohn’s disease | Ulcerative colitis, Crohn’s disease (extensive), FAP | Bladder cancer, spina bifida, neurogenic bladder |
In plain terms: If you have a colostomy, you’ve probably got it easier than ileostomy or urostomy patients in terms of output consistency and frequency. The trade-off is that your surgery likely involved cancer or significant disease. But the practical management of colostomy is, for many, more straightforward.
Learn more about how to manage each type in our comprehensive ileostomy guide and urostomy guide.
Surgery and Recovery
The Hartmann’s Procedure
If you had colorectal cancer affecting the rectum, you likely underwent a Hartmann’s procedure. This surgery removes the cancer-affected section of bowel (usually the rectum and part of the sigmoid colon) and creates a double-barrel colostomy: the functioning proximal stoma where stool exits, and a distal (or «mucous») stoma that’s left closed or may discharge small amounts of mucus from the rectum or distal bowel segment.
A Hartmann’s procedure is favored in many cases because it preserves the possibility of reversal—though reversal isn’t automatic and depends on factors like oncologic margins, radiation therapy, and your overall health.
The APR (Abdominoperineal Resection)
If you had an APR, the entire rectum and anus were removed. This is often necessary for cancers in the lower rectum. The result is a permanent end colostomy (typically sigmoid). There is no possibility of reversal with an APR because the anus is gone.
Recovery: What to Expect
Hospital stay: Usually 5-10 days. You’ll be monitored for infection, pain management, and beginning to tolerate food.
First 2-3 weeks: Rest, healing. Your ET nurse will teach you basic pouch care. Output may be unpredictable; this is normal. Pain and fatigue are significant. Avoid heavy lifting and strenuous activity.
Weeks 4-6: The stoma shrinks to its permanent size. You’ll be fitted with your correct pouch size. If you’re interested in irrigation, discussion and training begin now.
2-3 months: Most ostomates feel significantly better. Energy returns. Confidence with pouch changes increases. Irrigation (if you’re doing it) becomes more routine.
6 months: You’ve adapted. Colostomy life feels normal—not the life you planned, but manageable and increasingly invisible.
Emotional recovery takes longer than physical recovery. Cancer diagnosis trauma, fear of recurrence, and identity shifts don’t heal on the same timeline as your surgical incision. Support groups, counseling, and connecting with other ostomates accelerates this emotional healing tremendously.
Eating Well with a Colostomy
One of the best surprises for colostomy patients: you have more dietary freedom than ileostomy patients. Your colon, even partially, still absorbs water and some nutrients. You can eat most foods without restriction.
That said, certain foods warrant awareness:
- Gas-producing foods: Beans, cruciferous vegetables (broccoli, cabbage, Brussels sprouts), carbonated drinks, and artificial sweeteners can increase gas and potentially cause pouch ballooning or noise. Not forbidden—just something to manage.
- High-fiber foods: Whole grains, legumes, and some vegetables increase stool bulk, which is fine for most colostomy patients (especially irrigating ostomates). Some people find moderate fiber helpful; others with ascending colostomies might need to limit it.
- Odor-producing foods: Garlic, onions, eggs, fish, and certain spices can increase stool odor. Deodorants and odor-controlling foods (like parsley and yogurt) help.
- Speed-eaters beware: Swallowing large amounts of air or not chewing well can increase gas. Eat slowly.
- Alcohol and caffeine: Can increase output and gas; monitor your response.
There’s no universal «colostomy diet.» Keep a food diary for 2-3 weeks post-surgery to identify your personal triggers. Most ostomates quickly learn what works and what doesn’t, and then enjoy a diet that’s nearly unrestricted.
For detailed dietary guidance, see our colostomy-specific diet guide and broader ostomy nutrition guide.
Complications: What to Watch For
Most colostomies function without major complications, but some issues can develop. Early recognition and management prevent small problems from becoming big ones:
- Prolapse: The stoma tissue herniates through the opening and extends beyond the skin. It looks alarming (like a cherry or plum protruding from the stoma) but isn’t immediately dangerous. Can occur with loop colostomies or with straining/heavy lifting. Contact your surgeon; may require a supportive belt or, rarely, surgical repair.
- Hernia: A bulge around the stoma where the abdominal wall is weak. More common in obese patients, those with wound infections, or people who strain/lift heavily. Preventive measures: wear a supportive hernia belt, avoid heavy lifting, and manage constipation. Surgical repair is sometimes needed.
- Skin irritation: Pouch leaks allow stool to contact skin, causing redness and irritation. Ensure a good pouch seal, change pouches promptly if leaking, and protect skin with barrier products. Usually resolves quickly with proper pouch management.
- Stenosis: The stoma opening narrows, making output passage difficult and irrigation impossible. Can develop over months/years. Your surgeon may dilate it or, rarely, revise the stoma.
- Mucus discharge from distal stoma (Hartmann’s): The unused bowel segment produces mucus. A small amount is normal; excessive discharge can be managed by occasional irrigation of the distal stoma (consult your ET nurse). This doesn’t affect your colostomy function.
For detailed troubleshooting, consult our ostomy complications and troubleshooting guide.
Colostomy Reversal: The Hartmann’s Pathway
One of the most hopeful aspects of a Hartmann’s procedure: it can often be reversed. Not always, and not immediately—but reversal is possible, and many cancer survivors eventually choose it.
Is Reversal Right for You?
Reversal is considered after:
- Adequate cancer-free survival (typically 2-5 years, depending on cancer stage and recurrence risk).
- Successful completion of any needed chemotherapy or radiation.
- Clear imaging showing no recurrence.
- Good overall health and ability to tolerate a second surgery.
- Adequate anal sphincter function (the surgeon will test this with special studies).
- Your own readiness—reversal isn’t mandatory, and some ostomates prefer the predictability of their colostomy.
Not everyone is a candidate. Advanced cancer stage, poor sphincter function, or health conditions that make surgery risky may preclude reversal. Your surgeon will discuss candidacy honestly.
The Reversal Surgery
Reversal reconnects the proximal colon (the functioning part) to the distal colon or rectum, restoring normal bowel continuity. It’s typically a laparoscopic procedure (minimally invasive) and takes 2-4 hours. Hospital stay is usually 2-5 days.
Recovery is faster than the initial surgery because there’s less tissue trauma—you’re reconnecting what’s already there, not removing diseased bowel. Most people return to normal activity in 4-6 weeks.
After Reversal: Bowel Retraining
Here’s the reality: post-reversal bowel function isn’t identical to pre-cancer bowel function. Expect temporary (or occasionally, long-term) loose stools and increased frequency for the first few weeks to months. Your remaining colon and the new connection need time to adapt. Most ostomates see improvements over 3-6 months. Some experience occasional urgency or slightly looser stools permanently—but this is almost always manageable and much less disruptive than feared.
Dietary modifications (soluble fiber, adequate hydration, timing of meals) help optimize post-reversal bowel function. Many ostomates say the trade-off of slightly less-than-perfect bowel function for the independence of no pouch is absolutely worth it.
Reclaiming Your Confidence
A colorectal cancer diagnosis and surgery can shake your sense of identity and normalcy. You’re not just managing a medical device; you’re processing trauma, grief, and uncertainty. The practical questions (Can I wear this outfit? Will anyone notice? Can I exercise?) are real—but they’re also solvable. The deeper questions (Who am I now? Will my relationships change? Am I still whole?) take longer to answer, and they’re valid.
Work and Daily Life
Most ostomates return to work within 4-8 weeks. Your colostomy is invisible under regular clothing. With proper pouch management and occasionally a supportive ostomy belt, you can work in any environment—office, physical labor, healthcare, education. Disclosure to your employer is your choice and depends on your needs. Many ostomates work successfully without anyone knowing.
Exercise and Movement
You can exercise—truly. Running, weightlifting, yoga, swimming, cycling. The keys are supportive ostomy underwear or a belt for stability, secure pouching, and confidence. Swimming is possible: wear a waterproof pouch, or if you’re irrigating, wear a stoma cap and a rash guard for security and peace of mind. Check out our ostomy-specific swimwear.
Intimacy and Relationships
Sex, physical intimacy, and relationship dynamics shift after ostomy surgery—not always negatively, but they do shift. Communicate with your partner. Many ostomates find that after an initial adjustment period, intimacy actually deepens because vulnerability is met with acceptance. Wear a discrete pouch cover during intimacy if that helps you feel confident. Consider timing irrigation before intimate moments. Most importantly: your stoma is not disgusting or unlovable, and neither are you.
Travel
Travel is absolutely possible. Pack extra supplies (more than you think you’ll need), keep pouches in carry-on luggage, and research ostomy supply availability at your destination. If you’re irrigating, you can travel with portable irrigation kits. Time zone changes affect bowel output timing slightly; adjust your irrigation schedule gradually if traveling far.
Mental Health and Support
Consider connecting with support groups—online communities like the United Ostomy Associations of America (UOAA) or local in-person groups provide invaluable peer support. Talking to someone who’s lived it often matters more than any medical explanation. Some ostomates benefit from therapy, especially to process cancer trauma. This is normal, healthy, and available.
SIIL Products for Colostomy
Support and Confidence, Tailored for You
Managing a colostomy is about more than medical management—it’s about feeling secure, comfortable, and confident. Whether you’re newly adjusting or irrigation is in your future, SIIL ostomy accessories are designed by ostomates, for ostomates.
Our collection includes:
- Ostomy Support Belts — Discrete stabilization and hernia support
- Ostomy Underwear — Pocket support for active lifestyles
- Ostomy Swimwear — Swim with confidence
- Bag Covers — Discreet, stylish coverage
- Hernia Support Belt — Preventive support for vulnerable ostomates
- Ostomy Clothing Guide — Fashion tips for comfortable living


Frequently Asked Questions
Closing: A New Chapter, Not the End of One
A colostomy diagnosis arrived alongside fear, grief, and uncertainty. That’s real, and it’s valid. But sitting on the other side of surgery—even just a few weeks or months out—many ostomates discover something unexpected: a new normal that’s manageable, and in many ways, freeing.
You have control now. Irrigation gives you the power to schedule your body’s output instead of being surprised by it. Your diet is more flexible than you imagined. Your life—work, exercise, intimacy, travel—continues. It’s different from the life you planned, but it’s not diminished.
Colorectal cancer took something from you. But it didn’t take your future. With proper pouch management, support from healthcare providers and other ostomates, and acceptance that adaptation takes time, you’re building a full, confident life as a colostomy ostomate.
You’re stronger than you think. And you’re not alone.