Published on: 10/12/2025
Author: John Rainier Yumang
For many people living with a temporary colostomy, the idea of reversing it represents hope, normalcy, and a return to familiar routines. Colostomy reversal surgery, also known as colostomy takedown, reconnects the bowel internally so stool can once again pass through the rectum. While the procedure is common and often successful, it involves careful preparation, realistic expectations, and a recovery process that varies from person to person.
This guide brings together clinical insights from the Cleveland Clinic, Mayo Clinic, and the United Ostomy Associations of America (UOAA). It also includes helpful resources such as the SIIL Ostomy Ostomy Reversal Support Center, which provides educational tools and guidance for anyone preparing for either ileostomy or colostomy reversal.
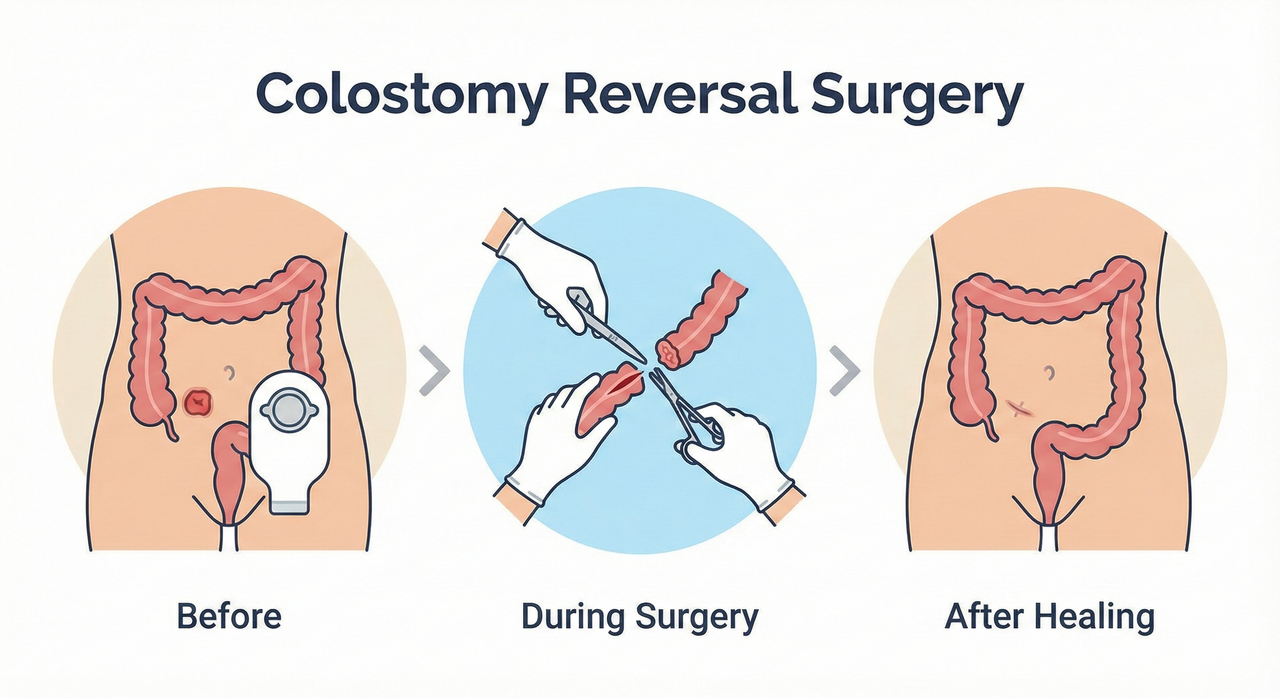
During the initial surgery that created the colostomy, the colon was brought through the abdominal wall to form a stoma. In colostomy reversal surgery, the surgeon reattaches the divided ends of the colon and closes the stoma site. The operation is generally shorter than the original one, but recovery can be more challenging because the bowel has been inactive and must re-adapt.
To understand the process in depth and explore preparation resources, the SIIL educational hub on ostomy reversal offers an accessible explainer page: learn more about ostomy reversal here.
Not every temporary colostomy can be reversed immediately. Surgeons evaluate several factors before recommending a takedown procedure:
According to the Mayo Clinic, the decision to reverse a colostomy depends heavily on whether the bowel has healed sufficiently and whether complications from the initial condition have resolved. Patients are often evaluated months after their original surgery, though timelines vary widely.
Preparation is just as important as the surgery itself. Patients preparing for colostomy reversal surgery may undergo:
For structured guidance, the SIIL Ostomy reversal guide offers step-by-step preparation support: reversal preparation guide.
Although every case is unique, colostomy reversal surgery typically follows these steps:
The procedure generally lasts one to three hours, and hospital stays range from two to five days depending on recovery progress. The Cleveland Clinic notes that bowel activity often remains unpredictable for days or weeks after surgery.
Recovery from colostomy reversal surgery involves both physical and functional healing. Patients may experience:
Because the bowel must relearn how to function, these symptoms are normal. Hydration, gentle dietary choices, and emotional support make a significant difference. For ongoing resources, SIIL’s information hub on ostomy reversal provides additional guidance.
Returning to daily routines takes patience. Surgeons commonly recommend:
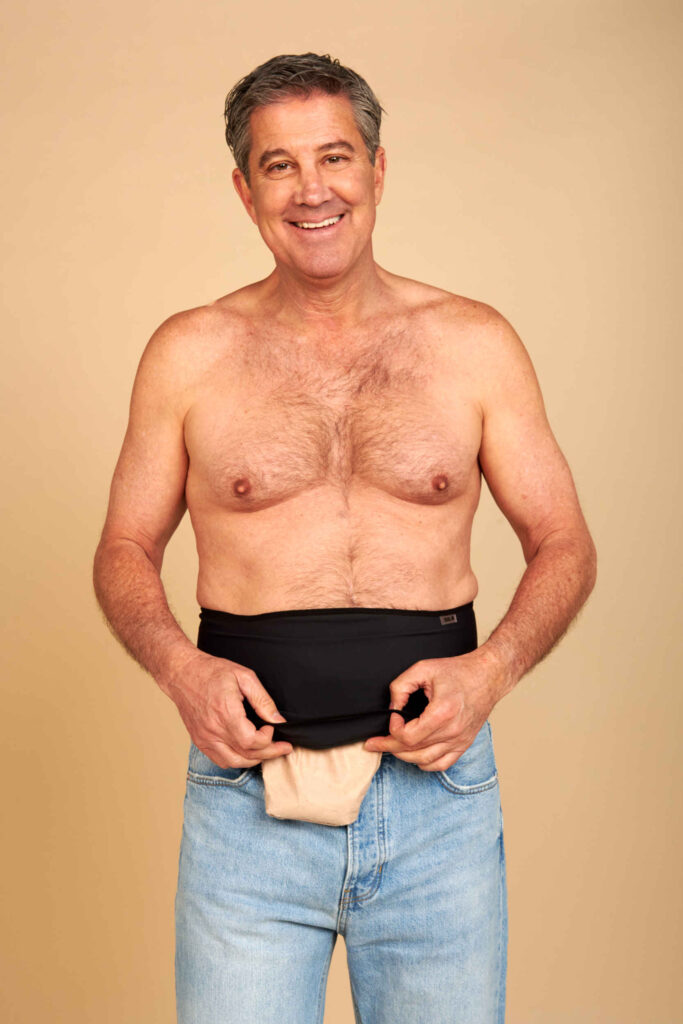
Some patients benefit from wearing supportive garments during early healing. These can provide confidence and gentle abdominal support:
While colostomy reversal surgery is generally safe, patients should be aware of potential risks:
Most complications can be managed successfully if detected early. For more postoperative care information, visit SIIL’s educational page on colostomy and ileostomy reversal.
Most patients experience steady improvement over weeks and months after colostomy reversal surgery. Long-term outcomes depend on the original condition, the quality of bowel healing, and the strength of pelvic floor muscles. While some individuals notice long-lasting sensitivity to certain foods, many return to stable and predictable bowel routines.
Most patients regain functional bowel habits within weeks, but full recovery can take several months.
Some discomfort is expected, but pain decreases significantly after the first few days.
Yes, most surgeons recommend gradually reintroducing foods while monitoring tolerance.
Complications such as infection or bowel obstruction may occur but are relatively uncommon when monitored properly.
The SIIL Ostomy reversal resource page provides ongoing support and guidance: Ostomy Reversal Information.
Share this with a friend:
DISCOVER MORE ARTICLES ABOUT OSTOMY
DISCOVER OSTOMY ACCESSORIES:
Author: María Gea Published: November 26, 2025 How to Wash
My Ostomy Bag Keeps Leaking, Causes, Fixes and When to
Be the Most informed Ostomate in the world.
Get updated about all the news about Ostomates, new tricks, tips, procedures, ostomy cards, traveling while getting in contact with the biggest ostomy community in the world.

Get Unique Offers and Discounts
Join more than 40.000 Ostomates worldwide in the SIIL Ostomy family and just profit from the offers, information and exclusive discounts just to be member.
41,99 €
50,00 €
29,99 €
41,99 €
46,99 €
49,99 €
38,99 €
100,00 €
89,99 €
59,99 €
49,99 €
29,99 €


We hate Spam as much as you do! Your email is safe here.

YOU'VE GOT
20% OFF
Sign up with your email to
claim 20% off sitewide!
